So I know I mentioned in my last post (Effects of Hearing Loss in case you haven’t caught up yet) that I would talk about handy tips and hints on how to improve communication for hearing impaired people and their family/friends, but I am going to deviate from my plan slightly as I have BIG (well, for me it is big anyway) news…
It has been confirmed that I will be having surgery for a Cochlear Implant on Thursday, as in 6 days away!! I had a meeting at the hospital yesterday to choose my device and have my final pre assessments done. It is exciting but nerve-wracking news. I was not expecting to receive an implant until 2015 but it looks like I will be starting the New Year in a positive way and with plenty of time for recovery and rehabilitation before I am due to tie the knot!
I wanted to focus this post on Cochlear Implants because I know a lot of people do not know that they are or understand their function fully and as I will most likely be rabbiting on about this topic for quite some time, I feel you should have some inkling of what I am talking about!
What is a Cochlear Implant (CI)?
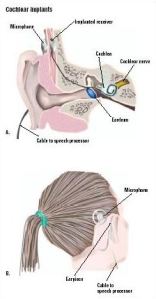
A CI is an electronic device that can assist those with severe to profound hearing loss. It is a surgically implanted device which is made up of an internal receiver and electrode array as well as an external speech processor that looks similar to a standard hearing aid.
Images from Surgery Encyclopedia and Speech – Hearing.com.
How do I get a CI?
As a single implant can cost upward of £25,000 there are stringent measures in place to determine suitability in the form of NICE guidelines.
You will need to have a referral to a CI centre from an ENT consultant or possibly even your GP.
An ENT consultant/audiologist will conduct several assessments such as speech perception, audiological and hearing therapy assessments and also liaise with you in regards to your personal expectations and motivation for having an implant.
After these tests, you will need to undergo medical assessments in the form of a surgical evaluation and CT and MRI scans. Once all this is complete a team of surgeons and audiologists will review your case and decide whether you meet the criteria for an implant and whether it is actually surgically possible as some are unable to have an implant due to middle ear problems or damage inside the ear. You will then meet with a consultant who will relay their decision to you.
Should you be accepted for a Cochlear Implant you will then need to attend pre assessment, chose your device (more on this in another post soon!) and have a meningitis vaccination.
How does a CI work?
The CI uses small electrical currents to directly stimulate the nerve of hearing which then sends signals to the brain where they are interpreted as sound.
Sounds from the environment enter the microphone which is located on the speech processor. The processor then selects and filters useful sounds; this information is then sent along the lead to the transmitter coil which is attached to the head using a magnet. The coil sends the information across the skin to the receiver/stimulator and this converts the information into an electrical signal. Pulses of electricity at the electrodes stimulate the hearing nerve which sends a signal to the brain to interpret the signal as a sound.
After the implant is put in place, sound will no longer travel via the ear canal and middle ear as is normal but will instead be picked up by the microphone and sent through the devices processor to the electrodes inside the Cochlea.
What kind of sounds can be heard with a CI?
This is subjective and varies across the board as every patients brain reacts and interprets sound differently. However, generally patients can usually hear and identify environmental sounds and find it helps improve their lip-reading – some can understand speech and use the telephone but this is not a guarantee.
Is it the same as “normal” hearing?
No. It is very different to normal hearing and has been described as “mechanical” and “electronic” sounding. As your brain adapts over weeks, months and years the sounds will become more natural to you. Music may not be accessible or enjoyable to all as CI’s are generally designed for processing speech.
Normal hearing relies on roughly 16,000 delicate hair cells and a CI has at most (device dependent) 22 electrodes to replace these.
It is important to understand that a CI is not and cannot “cure” deafness but it a prosthetic substitute for hearing.
What are the risks?
As with any type of surgery, there are potential risks. With this particular surgery there is an increased risk of contracting meningitis, so it is essential to be vaccinated against pneumococcal meningitis. There are also other risks such as facial paralysis and risk of anaesthetic. Your taste may also be temporarily disrupted with some patients describing taste as “metallic” immediately after surgery.
What happens during surgery?
The operation can take between 2-5 hours (depending on the chosen device and any other complications) and involves the receiver/stimulator being placed on the bone behind the ear and the electrodes being inserted into the cochlea.
A small area of the scalp directly behind the ear will be shaved and cleaned. Then an incision is made in the skin behind the ear and the surgeon will drill into the mastoid bone creating a small pocket for the receiver/stimulator and then into the inner ear where the electrode array is inserted into the cochlea.
Will I be able to hear immediately after surgery?
No. The wound behind the ear where the receiver/stimulator and electrodes have been inserted needs to fully heal before any external parts can be worn. Patients generally don’t receive external parts until about 4 weeks after surgery.
What happens when you are “switched on”?
There will be a tuning process whereby the speech processor is adjusted to suit your needs, this involves audiological tests to see what sounds can be heard. Tuning sessions will need to be carried out every couple of weeks for the first few months as you will be switched on in stages.
You may not be able to identify any sounds immediately after switch on, some patients described hearing lots of beeps and whistles with voices sounding robotic or chipmunk like. Your brain will need time to adapt to the different sounds being processed.
What happens if I am not accepted for a CI?
If for some reason, you do not meet the NICE guidelines for a CI, the NHS will refuse to offer you an implant. However, most hospitals will re-evaluate you in approximately 6 months to see if your hearing has changed, even if it has changed only slightly, it may assist your case. You can ask your audiologist to refer you to a different hospital if you feel this is appropriate.
I was initially refused a CI from the first hospital I went to and it was heartbreaking for me and my family. The hospital concerned did not feel that I could be classed as an “exceptional circumstance” so our appeals were rejected. I was fortunate in that I had an audiologist (and mum) who refused to give up on this and so I was referred to a second hospital who, as you can tell from this article, have accepted me! Had they not, the next step would have been referral to a hospital in Nottingham!
The important thing to remember is do not give up!!
I hope this post has been helpful and has helped you to understand a little more about CI’s, if there are things you are uncertain about or you just want to learn more, check out the British Cochlear Implant Groups website http://www.bcig.uk.
Please bear with me over the coming weeks and months, I will be a bit of a hermit after my operation as I am unable to leave the house (or even wash my hair, eugh!) for about two weeks due to risk of infection. It does mean over the Christmas period I will be very quiet but hopefully with switch on in the New Year, I will be back to my old self!
Roll on 2015!



So pleased to find your blog. Had implant fitted on 29 Feb 2016 so 5 days ago. Still sore but very optimistic. My journey similar to yours but in Wales once accepted you have to wait up to 52 weeks for implant. I waited 56 weeks and intend to campaign to get better results for people in Wales. After the journey through referrals and assessments it will have taken over 4 years of visits to different audiologists, consultants and surgeons so not an easy journey. Like you I appealed first decision to refuse implant especially as it was so very close. There are only audiology grounds for acceptance with no or little consideration of social impacts for adults. My argument is that adults suffer greater social impacts than children especially with work and emotional impacts of losing or leaving a job because of hearing loss. It is more difficult to get employment and support is becoming more difficult to attain.
Switch on for me is 11 April. I have some hearing (bordering on profound) in my ‘good’ ear and have some residual support from a good private aid. My right ear (where the implant is) has no hearing and the impact from the operation has been nil so on that basis whatever happens now I have lost nothing.
I will read other blogs and will try to write more myself. It has been such a rollercoaster week as nearly had operation cancelled due to lack of bed. But everything is coming right now.
Jackie Charlton – Optimistic Cochlear Implant recipeint
5 March 2016
LikeLike
Thank you for taking the time to comment on my post – I love to hear other people’s stories.
I hope the implant works well for you – if you ever want some advice/rehabilitation tools I would be happy to send you some.
I’m horrified you had to wait 56 weeks to get the implant, that is simply not good enough, I fully support your future campaign and if I can ever lend support in some ways I would be happy to do so.
I do agree with your argument regarding the social, emotional and professional impacts that hearing loss has on adults and find it frustrating that the NICE guidelines do not recognise this.
I wish you all the best for your switch on in April and would love to hear how you get on!
Laura Lowles
LikeLike